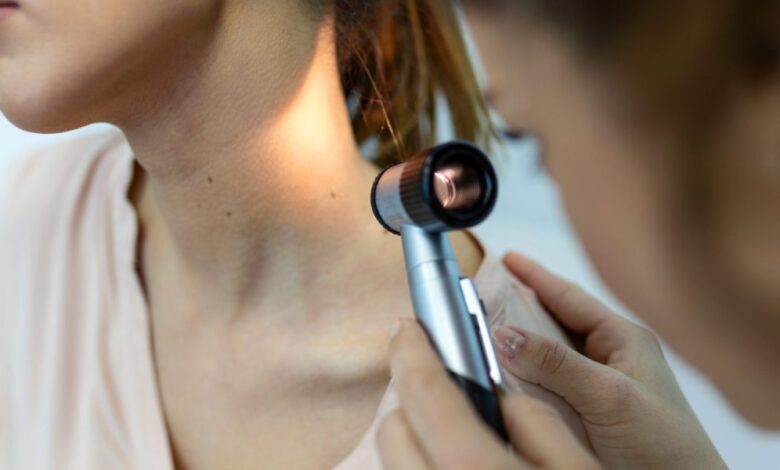

Protecting oneself from the summer sun and its damaging ultraviolet rays is often not straightforward. And public health messaging around when and how to be screened for skin cancer has become somewhat confusing.
In April 2023, the U.S. Preventive Services Task Force, an independent national panel of science experts, provided updated recommendations on skin cancer screening following a systematic review of existing research. The task force concluded that the evidence does not support annual widespread skin screening of adolescents and adults, but that catching cancers at the earliest stages reduces the risk of death from skin cancer.
At first glance, these statements appear conflicting. So The Conversation asked dermatology experts Enrique Torchia, Tamara Terzian and Neil Box to help unravel the task force recommendations, what they mean for the public and how people can minimize their skin cancer risk.
How common is skin cancer in the US?
Skin cancer affects about 6 million Americans yearly, according to the Centers for Disease Control and Prevention. This number is more than all other types of cancers combined.
Basal cell carcinoma and squamous cell carcinoma – collectively known as keratinocyte cancers – account for more than 97% of skin cancer cases, but invasive melanomas cause the most deaths. Keratinocyte cancers arise from basal cells and the more differentiated squamous cells in the epidermis – the top layer of skin – whereas melanoma comes from melanocytes found at the junction of the epidermis and the dermis, or middle layer.
Unlike normal cells, skin cancer cells grow without constraints, acquiring the ability to invade down into the dermis.
Invasive melanomas are classified by stages 1 through 4. The higher the number, the more invasive the tumor is into the dermis and to other organs of the body in a process called metastasis.
What are the main causes of skin cancer?
Overexposure to ultraviolet rays causes the majority of skin cancers. Both light- and dark-skinned people can get skin cancer, but light-skinned individuals have a greater risk. Those with light skin, light or red hair, or with numerous moles, are more susceptible to skin damage and severe burns by ultraviolet rays. Darker-skinned individuals produce more of the protective pigment called melanin.
Tanning serves as the body’s protective response to skin damage from ultraviolet rays, stimulating melanocytes to produce melanin. People who use tanning beds are at a higher risk of skin damage and skin cancers. This is why the American Academy of Dermatology and others recommend avoiding tanning beds. Outdoor workers or those who spend time outdoors recreationally, especially at higher elevation, are exposed to more ultraviolet light.
A history of sunburns also puts people at greater risk of developing skin cancer. Because the damage from ultraviolet, or UV, exposure is cumulative, skin cancer is more prevalent in people over 55 years old.
Survivors of skin cancers are also more likely to get another cancer in their lifetime. Moreover, those who had a squamous cell carcinoma may be at higher risk of dying from noncancer causes. The reasons for these observations are not well understood but may be linked to inflammation or altered immunity, or both, in skin cancer survivors.
What is the debate behind screening?
The ongoing debate revolves around whether more screening reduces the death toll from melanoma.
Since the early 1990s, the incidence of melanoma has risen dramatically in the U.S. This increase may be due in part to more emphasis on early detection. More melanomas have been found, particularly those identified at the earliest stage, also known as stage 0 or melanoma in situ.
Despite this, the rate of death per capita from melanoma has remained unchanged over the last 40 years. Researchers have attributed this fact to overdiagnosis, in which suspicious lesions are diagnosed as early melanomas, even though they may not actually be melanomas or progress to be invasive melanomas, which have the worst prognosis.
This observation suggests that widespread screening may result in unnecessary surgical biopsies and increased psychological stress associated with a cancer diagnosis.
However, a recent study published after the task force recommendations showed that patients with melanoma in situ had a slight risk of death from melanoma, but lived longer than the average person. The authors speculated that the diagnosis of early stage melanoma resulted in a greater awareness of the patient’s overall health, leading to more health-conscious behavior. So, there may be additional benefits to screening the public.
What did the task force base its new recommendations on?
The task force reviewed current and past data on the major types of skin cancers. The expert panel relied in part on the results of a large public skin cancer screening program in Germany. This program initially examined 20-year-olds from a single state and subsequently expanded the program nationwide to include people over 35. However, death rates from melanoma were unchanged compared to areas where skin exams were not offered.
The results of the German screening program did not provide strong confidence that annual widespread public screening of adults would reduce skin cancer deaths compared with current practices. However, the task force did conclude, based on numerous studies involving millions of patients, that detecting melanoma at early stages when tumors are less invasive improved patient survival.
When should you get a skin exam?
The American Academy of Dermatology, the Skin Cancer Foundation and the CDC recommend monthly self-checks. This requires familiarity with your skin or that of your family members. Luckily, there are many online guides on detecting suspicious skin lesions.
Whenever you have a concern about a spot on your skin, seek medical advice. Annual or more frequent exams are also recommended for high-risk groups. This includes those who are older or susceptible to getting skin cancers, skin cancer survivors and immunocompromised people like organ transplant recipients.
Between 8% to 30% of the U.S. population gets an annual skin exam, but the numbers are imprecise because screening rates have not been well studied. Access to screening may also be challenging for some people. In response, nonprofits like the American Academy of Dermatology, the Skin Cancer Foundation and The Sun Bus provide resources for free exams. However, these opportunities are often few and far between.
Based on internal unpublished data from The Sun Bus, our mobile clinic operating in the central and southern U.S., a significant number of individuals seeking free exams were primarily motivated by concerns about a skin lesion and the cost of visiting a dermatologist.
Our data suggests that screening programs attract individuals who are proactive and health-conscious.
How can you minimize the risk of skin cancer?
Strategies that limit UV exposure will reduce skin cancer risk. This includes avoiding sunburns by:
- Finding shade
- Covering exposed skin
- Using a hat and sunglasses
- Using and reapplying sunscreen routinely
A broad-spectrum sunscreen and lip balm with a Sun Protection Factor (SPF) of at least 30 when applied correctly will block 97% of ultraviolet rays. Apply these products 15-20 minutes before heading out into the sun and reapply every two hours.
UV light is most intense between the hours of 10 a.m. to 4 p.m. It is a good idea to pay attention to the UV index – a forecast by zip code that projects risk of UV exposure on a scale of 0 to 11. A UV index below 2 is the safest, whereas 11 represents extreme danger.
Ideally, clothing should be rated with an Ultraviolet Protection Factor (UPF) of 50. Wearing regular long-sleeved clothing and pants will also provide some protection.
These measures can keep your skin healthy into your golden years by reducing skin aging and cancer caused by ultraviolet light.
Enrique Torchia, Assistant Research Professor of Dermatology, University of Colorado Anschutz Medical Campus; Neil Box, Associate Clinical Professor of Dermatology and Epidemiology, University of Colorado Anschutz Medical Campus, and Tamara Terzian, Assistant Professor of Dermatology, University of Colorado Anschutz Medical Campus
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Source link




